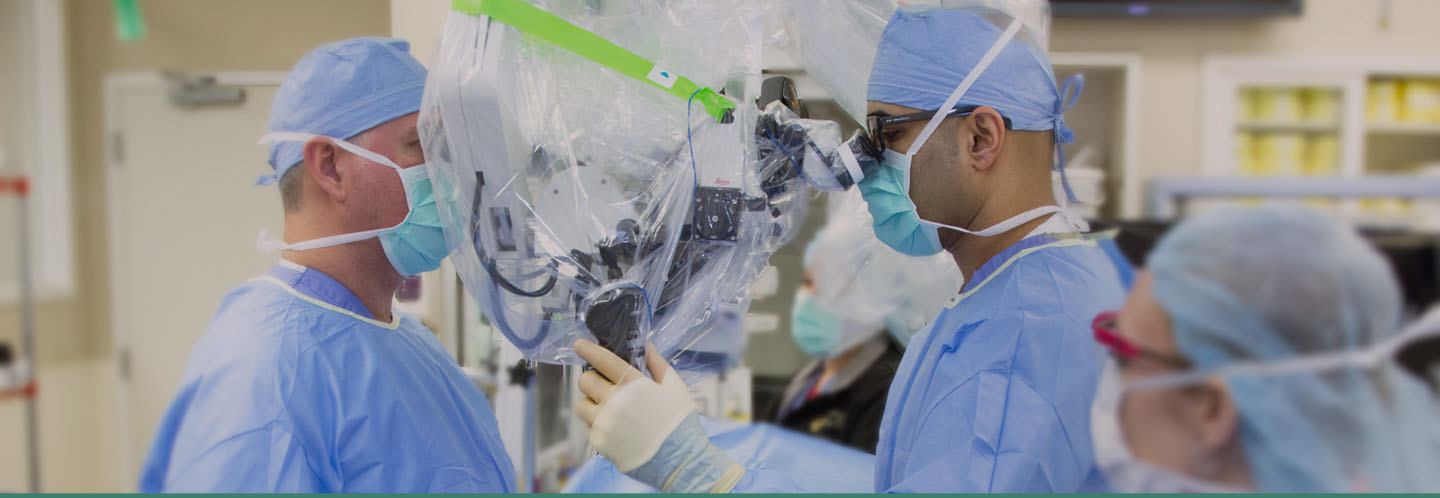
Vasectomy Reversal in Chattanooga, TN
Can A Vasectomy Be Reversed?
Women have many choices for birth control. Men only have one effective form of birth control, the Vasectomy. Vasectomies are considered permanent. But, circumstances can change. About 5% of men with a vasectomy choose to have it reversed. The only way to regain the ability to conceive a child naturally through intercourse after vasectomy is by a vasectomy reversal. It also tends to be the most cost-effective way to have a child after vasectomy compared to IVF and sperm retrieval.
Dr. Shridharani is a high volume microsurgeon who has fellowship training in male reproductive microsurgery. This means that he offers the best vasectomy reversal success rates, and will discuss with you all of your options to get pregnant after a vasectomy. Dr. Shridharani offers Vasectomy Reversal’s in Chattanooga, TN but often see patients from areas like Nashville, Knoxville, Northern Georgia & Huntsville, AL.
How Much Does A Vasectomy Reversal Cost?

Does Insurance Pay for a Vasectomy Reversal?
We understand the significant cost that is associated with having a child after vasectomy. Although some insurance plans cover reversals, most do not. Nevertheless, we will assist you in the process of readying your claim for submission. Sometimes, insurance will cover parts of the cost, such as the anesthesia and facility fee. I feel it my practice’s responsibility to help you through this process since it can be time-consuming, frustrating and costly. I will do my best to provide the necessary information to get your claim approved. I do recommend all interested parties submit a claim to minimize cost. The claim submission and review process is outside the scope of our practice, and unfortunately, we do not have direct control of claim outcomes.
Click Here For Pricing
VASECTOMY REVERSAL FAQS
THE VASECTOMY REVERSAL PROCEDURE
Vasectomy reversal is a relatively simple surgery. The objective is to restore the flow of sperm. The success of a reversal is based on two things, patency, and pregnancy. Patency is the surgical success rate, or the ability of the procedure to successfully restore sperm in the ejaculate. However, getting sperm into the ejaculate does not guarantee pregnancy which is more dependent on the fertility status of the female partner. Pregnancy rates vary from 30-70% based on the patency rate and female fertility status.
- The procedure is usually done on an outpatient basis under general anesthetic and takes between 2-4 hours. Dr. Shridharani does not perform the procedure under a local anesthetic because that prevents the ability to perform a more complex connection if necessary.
- He uses a microscope to make tiny incisions that will suture the cut ends of the vas deferens together. During surgery, the presence of sperm at the cut end of the vas deferens will be confirmed.
- If there is moving sperm or the quality of the fluid exiting the vas is good, a connection can be made. This procedure is called a vasovasostomy (VV) or vas to vas connection. When this type of connection is performed patency rates are usually about 85% if performed on one side and 90+% when performed on both sides.
- If no sperm parts are found or the quality of the fluid is poor like toothpaste, it is likely there is a blockage closer to the testicles, which may require a more complicated connection.
- The connection usually involves connecting the vas deferens to the epididymis, the structure on the back of the testis that allows sperm to mature. This connection is called an epididymal-vasectomy (EV) and is usually associated with lower patency rates because the tubes being connected are extremely delicate and small, about the size of a ridge of your fingerprint. This particular connection requires the use of an operating microscope and most of the surgeons able to do this have fellowship training due to its complexity.
- The incisions are usually closed with sutures that will dissolve over time. The size of the incision depends on the connection that is made.
- Although the incisions are generally small, 1-3cm in size, Dr. Shridharani will not let the size of the incision impact success rates. If you require a larger incision or additional incision to maximize your chance of success it will be done.
Contact Dr. Shrid to Schedule an Appointment
WHAT IS THE VASECTOMY REVERSAL RECOVERY LIKE?
I perform vasectomy reversals predominantly on Friday morning so many men can return to work on Monday. Men who have jobs that require manual labor or heavy lifting are able to return after a week, or sooner if work restrictions are allowed. Men will experience swelling, bruising and discomfort. However, most men when sitting at rest after the procedure will be comfortable. Recovery takes about 2-3 days. You will be advised to use ice packs and scrotal support. You can return to work within 2-3 days if you do not have a requirement for manual labor. I suggest refraining from sexual activity for 3 weeks, and not to engage in vigorous activity/exercise until about 7-10 days post-operatively. Most couples have invested significant time and energy by the time they undergo a reversal and therefore, it is imperative that they take care of the surgical sites as if their pregnancy depended on it. Any job requiring heavy lifting should be postponed for 2-3 weeks after reversal.
I will guide you through the process and help you determine the best post-vasectomy fertility option to help you have a child. I have devoted my practice to assisting couples to get pregnant through medicine and surgery. I perform microsurgery and reversals on a regular basis and I am comfortable performing the most complex of vas reconnections to optimize your chances of achieving pregnancy. I promote couple involvement in all aspects of the decision-making process and find this empowers couples and improves satisfaction overall.
I’M PRETTY OLD OR HAD PROBLEMS WITH MY VASECTOMY, AM I STILL FERTILE?
Before surgery, your surgeon will confirm if you are fertile. He will examine you for testicular health, testicular disorders, blockages and abnormalities of the vas deferens. All these factors determine what your fertility status is and what it will be post procedure. Dr. Shridharani has performed successful reversals in men over the age of 50. Men of advanced age will usually have additional hormonal testing in the pre-operative period to confirm testicular function.
If you are on testosterone therapy, or anabolic steroids you will need to be off the hormones for at least three months before the procedure. Testosterone that is artificially given can suppress your normal production of sperm and one has to be off the drug for several months to allow the recovery of sperm production prior to the reversal. This is very important. Any usage of testosterone in close proximity to the procedure can impact the reversal procedure and success rates.
WHAT OTHER CONCERNS SHOULD I HAVE?
- Scarring can occur any time after the procedure, but it usually happens within the first 6 months. It is possible that scarring can lead to blockage and infertility. For this reason, we offer sperm banking with the vasectomy reversal. Getting semen analyses at regular three-month intervals is important to identify the presence of scarring unless pregnancy occurs indicating fertility. Scarring can usually be treated to allow adequate amounts of sperm to return to the ejaculate during pregnancy.
- 70-80% of men who have vasectomies will have antibodies to their sperm. But this rarely prevents the sperm from fertilizing the egg. The presence of anti-sperm antibodies do not change anything and therefore is not concerning to your surgeon.
- Sperm quality and count usually improve over time. If your first semen analyses show small numbers or poor quality that is to be expected and will likely improve over time.
Contact Dr. Shrid with Questions or Concerns
WHAT ARE ALL OF THE POST-VASECTOMY TREATMENTS OPTIONS?

- Vasectomy reversal with or without sperm retrieval
- Sperm retrieval for use with IVF
- Intrauterine insemination with donor sperm
- Adoption
MY PREVIOUS VASECTOMY REVERSAL FAILED, WHAT ARE MY OPTIONS?
All of the post-vasectomy options are open for you to pursue. Redoing the vasectomy reversal offers similar success rates to the original reversal as long as your underlying fertility can be confirmed. Dr. Shridharani can discuss these options with you further during your consultation.
Dr. Shridharani will guide you through the process and help you determine the best post-vasectomy fertility option to help you have a child. Dr. Shridharani is primarily a male reproductive surgeon. His practice is devoted to assisting couples to get pregnant through medicine and surgery. He is a high volume microsurgeon and is comfortable performing the most complex of vas reconnections to optimize your chances of achieving pregnancy.
He has authored a study on Vasectomy Reversal Best Practices based on high volume microsurgeries and maintains a contemporary, up-to-date practice based on ASRM and AUA recommendations. Of the utmost importance, Dr. Shridharani will counsel you on all of the options and help find the treatment option that is cost-effective and agreeable to you and your partner. We promote couple involvement in all aspects of the decision-making process and we find this empowers couples and improves satisfaction overall.
See What Our Patients Are Saying…“I would highly recommend Dr. Shridharani to anyone. I was referred to him by another doctor in his field because of the complicated nature of my case, and was told that Dr Shridharani was the best physician to address my surgical needs. From the first time I met him, he was very thorough and very patient with me. He spent as much time as I needed to answer my questions and explain all of my options. I am very pleased with my outcome and thankful there is a specialist of his caliber here in town. It is nice in todays world of “quick” medicine to find someone who takes the time to address your concerns and needs.” – B.B.
I’VE HEARD VASECTOMY REVERSALS ARE NOT SUCCESSFUL, IS THAT TRUE?
In general, the answer is no, reversals are very successful. However, multiple factors can affect the success of a reversal. Achieving surgical success or patency allows for sperm to return to the ejaculate to increase the chance of pregnancy naturally. Surgical success is dependent on multiple factors such as how long ago the vasectomy was performed, whether there is sperm present at the cut end of the vas at the time of reversal, and the experience and training of the surgeon performing the reversal.
Achieving pregnancy, which is what most couples are looking for, is dependent on the presence of sperm in the ejaculate after reversal, and the fertility status of the female partner.
Generally, surgical success/patency is achieved in 90+% of patients and pregnancy can be expected in 60-70% of patients. Nevertheless, these numbers are not guaranteed for everyone undergoing reversal. Your male reproductive vasectomy reversal specialist should individualize the success rates for you based on the factors noted above.
Click to Call Dr. Shrid Today to Learn More
I HAD MY VASECTOMY OVER 20 YEARS AGO. WOULD MY REVERSAL STILL BE SUCCESSFUL KNOWING THAT?
Vasectomies can be reversed after long periods of time as men continue to produce sperm throughout their lifespan when healthy. I have performed multiple vasectomy reversals in men who have had their vasectomies done 25 years or more previously, with good success and subsequent pregnancy. However, the likelihood that your vas reversal surgeon will have to perform a technically challenging vasoepididymostomy(EV) is higher.
When an EV is performed the success rates overall are slightly decreased compared to a vasovasostomy (VV) which is less challenging. Most surgeons who are able to perform an EV when appropriate are fellowship trained in male reproductive microsurgery. Your surgeon will offer you counseling about whether your chance of pregnancy would be better served with vasectomy reversal versus other forms of achieving pregnancy after vasectomies, such as sperm retrieval and in-vitro fertilization.
DOES THE TYPE OF VASECTOMY AFFECT THE OUTCOME OF THE REVERSAL?
Not usually. Vasectomies, with regard to the technique used, including the use of cautery, surgical clips or ties, have little bearing on the outcome of the reversal. The surgeon performing the reversal should have enough experience to navigate the minor and major changes in anatomy related to the vasectomy to offer you the best possible outcome. The time from vasectomy, the presence of sperm at the time of reversal and the fertility status of the female partner has more bearing on success than the type of vasectomy performed.
I HAVE HAD TESTICULAR PAIN EVER SINCE MY VASECTOMY. WILL THE REVERSAL CURE MY PAIN?
The causes of testicular pain are many. A thorough evaluation of your pain, including a history and physical exam, will be performed. Some people who have pain related to a blockage of the vas deferens, once confirmed by your physician, may benefit from a reversal. The likelihood of pain resolution with reversal will be discussed at your visit based on your assessment.
WHO IS NOT A CANDIDATE?
Men who have undergone a vasectomy, with partners who have undergone tubal ligation, may not be best served by vasectomy reversal alone. Tubal reversal for the female partner will be required along with vasectomy reversal to allow for natural conception. The best options for couples in this situation may be in-vitro fertilization and sperm aspiration to achieve pregnancy. Sperm aspiration may be done under a local anesthetic via TESA and is well tolerated in general with minimal if any recovery.
Contact Dr. Shrid to Schedule an Appointment
WHAT ARE THE SIDE EFFECTS OF THE VASECTOMY REVERSAL?
Postoperatively, men will experience discomfort at the incision and possibly at the site of the vasal anastomosis (where the connection of tubes was made). Bruising and minor swelling is also expected. The sutures used to close the incisions do not require removal and the incision size depends on the type of connection being made. If the vasectomy was done high in the scrotum and you require a vasoepididymostomy (EV) there is a chance that the testis will ride higher on that side compared to pre-operatively. Your surgeon will address this issue prior to the operation to alert you if this may be an issue. Change in sex drive, erections or urination are not to be expected after the reversal. Although there have been reports of increased cancer risk for men undergoing a vasectomy, this evidence has not been confirmed. Performing vasectomy reversal does not carry any cancer risk.
HOW IS SURGICAL SUCCESS OR PATENCY ASSESSED AFTER THE REVERSAL?
After a VV, a semen analysis is checked at 6 weeks. After an EV on both sides, the semen is checked at three months. The difference in interval has to do with the normal turnover of sperm which occurs between 2 and 3 months. If there is sperm present in any amount the patency or the “openness” of the connection is confirmed. If your partner gets pregnant prior to the semen analysis, which is very possible and does not occur infrequently, then the assumption that your connections are open is made.
ARE THERE OTHER MEANS OF “FERTILITY” THAT I SHOULD CONSIDER INSTEAD?
At the time of your consultation whether in the clinic, or over the phone, all of your post-vasectomy options will be reviewed. There are multiple ways to have a child. The only way to have a child naturally through intercourse is via vasectomy reversal. Another way to obtain pregnancy is through in-vitro fertilization. Sperm, since not present in the ejaculate, will have to be surgically retrieved via (TESA or MESA). The sperm used will be injected into the egg, and the healthy eggs will be implanted into the uterus after the female partner has taken hormone injections.
A female reproductive specialist coordinates the in-vitro fertilization process, and our practice has partnered with several excellent specialists in the region to offer this service when requested. The pregnancy rates of IVF are comparable to vasectomy reversal when averaged over three IVF cycles. The cost-effectiveness of vasectomy reversal over IVF has been substantiated in the literature and depends on several factors that can be discussed by your surgeon.
The other two ways to obtain a child are through artificial insemination of the woman, with the use of donor sperm and through adoption. Sperm retrieval from the man that has undergone vasectomy does not usually amount to that required for artificial insemination but is fine for IVF.
Click to Call Dr. Shrid Today to Discuss Your Options
WHAT ARE ANTI-SPERM ANTIBODIES, AND WILL THOSE AFFECT MY CHANCES OF GETTING PREGNANT?
Since the sperm is not completely immunologically identical to the rest of the cells within the body, theoretically the body can fight and kill sperm. There is an overwhelming prevalence of anti-sperm antibodies in men that have undergone a vasectomy. However, the presence of these anti-bodies bears little to no influence on the outcome after reversal. Therefore, I do not test or recommend testing for anti-sperm antibodies as a routine practice.
WHEN CAN SCARRING OCCUR?
Scarring can occur anytime and can be classified as early or late scarring. The scarring process is dependent on what type of connection was made (EVs tend to scar more), the surgeon’s training and experience, trauma or infection, and other patient factors. As stated previously, obtaining semen analyses post reversal is important in treating scarring prior to complete blockage of the connection. It is often difficult to determine the inciting factor that led to the scarring and can be a frustrating experience for the couple. Up to 10% of men undergoing reversal can have scarring found, up to two years post-procedure.
When a semen analysis reveals smaller amounts of sperm that is necessary for conception, sperm banking will be recommended for fertility preservation. Banked sperm can be used for intrauterine insemination or in-vitro fertilization, depending on the amounts and mobility of sperm collected.
WHAT HAPPENS IF NO SPERM IS FOUND DURING THE PROCEDURE?
Sperm in the fluid where the vas deferens is cut can be a predictor of success. However, several scenarios exist when no sperm is found. If a knot is present at the end of the vas deferens and is identified on physical exam, it could signify a sperm granuloma. Usually, sperm granulomas are a good sign because they indicate less backpressure on the epididymis and testis over time. Also, if plenty of clear fluid is seen without sperm present that also is a good sign and a VV can be made.
However, if a thick fluid is found without sperm, or no fluid is found and there is no sperm granuloma, the structure on the back of the testis will need to be explored. Often dilated tubules and/or a blockage will be present and an EV will be performed. Due to the training and experience required to perform an EV, you should seek a surgeon that will discuss these issues with you, prior to the procedure. With an EV, the incision may also be larger. I do not let the size of the incision influence my goal of maximizing your chance at pregnancy and will always perform an EV when appropriate.
HOW DO I ASSESS WHETHER MY SURGEON WILL OFFER US THE BEST CHANCE OF PREGNANCY?
This question is often the most difficult for patients and can be frustrating. I was involved with a study that identified the criteria that are best practices for a vasectomy reversal. First, all the post-vasectomy options to obtain a child should be reviewed with every couple prior to choosing a plan. Surgeons who offer vasectomy reversal as the only option after vasectomy do a disservice to patients. Next, fellowship training in male reproductive microsurgery is recommended, although there are exceptions. There are several, albeit few, microsurgeons who pioneered the field prior to fellowships being available.
Nowadays, the skill and training necessary are only provided by fellowships, where leaders in the field train surgeons to be not only technically proficient but to offer the complex individualized assessment and counseling that patients deserve prior to treatment. Next, your microsurgeon should offer their surgical success rates and pregnancy rates, as well as how often they perform the procedure. Use of an operating microscope, and being able to perform a 2-layer anastomosis is necessary to perform an EV. The vasal fluid should also be sampled and examined in the operating room since they are the main indicators of when to perform an EV.
WHAT CAN I DO BEFORE THE VASECTOMY REVERSAL TO MAXIMIZE MY CHANCE OF SUCCESS?
For most people there is not much you need to change prior to the reversal to improve your success rates. Nevertheless, testosterone therapy in the months prior to the reversal is an absolute reason to delay the reversal to a later date. Often testosterone therapy does not help your fertility status and can decrease your sperm count to zero. This is a potential problem because the presence of sperm at the time of surgery is the main indicator of what type of connection is made. Usually, men who are on testosterone therapy that are seeking a vasectomy reversal are recommended to stop their testosterone and are placed on other medication.
Schedule a Consultation For A Reverse Vasectomy in TN
Dr. Shridharani proudly serves Chattanooga, Nashville, and Knoxville, TN as well as the surrounding areas in Northern Georgia, and Huntsville, AL. Dr. Shridharani is the best choice when it comes to his advanced vasectomy reversal techniques. Call (423) 778-4MEN (4636) to schedule an appointment today! Or, click here to send our office a consultation request form. We look forward to serving you!